|
|
|
|
|
To
Main Page
To
PRP - Prolotherapy
Directory
|
P.R.P & Prolotherapy
Article Written By:

Dr. Donna Alderman
Medical Director
Hemwall Center for Orthopedic Regenerative Medicine
http://www.prolotherapy.com
info@prolotherapy.com
28212 Kelly Johnson Parkway Suite 135
Valencia, CA 91355
Tel: (661) 295-1110
or (818) 957-3000
|
To Main Page
About BMOTV™
|
|
About BMOTV™
|
Platelet
Rich Plasma (PRP) and Prolotherapy
What is it?
Can it heal soft tissues and bones
in humans & animals?
|
|
|
To
Top
|
|
To
Top
|
|
|
Platelet Rich Plasma (PRP) Prolotherapy, like Dextrose
Prolotherapy,
is a method of injection designed to
stimulate healing. “Platelet rich plasma”
is defined as
“autologous blood with concentrations of platelets above
baseline levels, which contains at least seven growth
factors.”
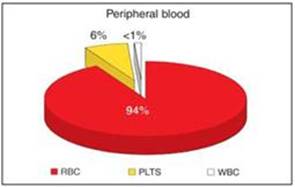
Cell ratios in normal blood contain only 6%
platelets, however in PRP
there is a concentration of 94%
platelets. Platelets contain a number of proteins,
cytokines and other bioactive factors that initiate and
regulate basic aspects
of natural wound healing.
Circulating platelets secrete growth factors,
such as
platelet-derived growth factor (stimulates cell
replication, angiogenesis),
vascular endothelial growth
factor (angiogenesis),
fibroblast growth factor
(proliferation of myoblasts and angiogenesis),
and
insulin- like growth factor-1 (mediates growth and repair
of skeletal muscle),
among others. Enhanced healing is
possible when platelet concentration
is increased with
PRP. Activated platelets “signal” to distant repair cells,
including adult stem cells, to come to the injury site.
Increasing the volume
of platelets accordingly increases
the subsequent influx of repair and stem cells.
Because
the concentrated platelets are suspended in a small volume
of plasma,
the three plasma proteins fibrin, fibronectin,
and vitronectin contribute
to a repair matrix. You could
compare dextrose Prolotherapy
and PRP this way:
Prolotherapy is like planting seeds in a garden;
PRP
Prolotherapy is planting seeds with fertilizer.
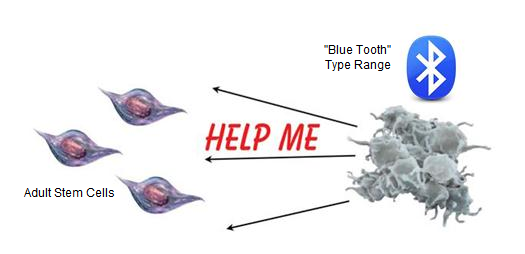
PRP mode
of action: Activated platelets signal for
help
from local repair stem cells.
|
|
|
To
Main Page
|
HISTORY
OF PLATELET RICH PLASMA THERAPY
(PRP)
|
To
Main Page
|
|
|
|
|
|
|
Beginning in the 1990s and continuing
until now,
“growth factors” have been a hot topic in the medical world.
It is clear that
growth factors play a pivotal role in all types of wound healing.
Investigation into
the use of PRP has been reported as early
as the 1970s, but the necessary equipment was large,
expensive
($40,000 in 1996), and required a large quantity of a patients blood (450 cc)
and therefore limited to the operating room for large scale surgeries.
Starting
in the early 1990s, multiple reports and studies
in maxillofacial dental,
periodontal surgery, cosmetic surgery,
and skin grafting showed dramatically
improved healing with PRP.
In the early 2000s, the use of PRP expanded into
orthopedics
to augment healing in bone grafts and fractures. Success
there encouraged
its use in sports medicine for connective tissue
repair. Mishra and Pavelko,
associated with Stanford University, published the first human study
supporting the use of PRP for chronic tendon problems in 2006.
This study
reported a 93% reduction in pain at two year follow up.
Then, in 2008,
Pittsburgh Steelers’ wide receiver,
Hines Ward, received PRP for a knee medial collateral
ligament sprain,
and the Steelers went on to win SuperBowl XLII. Ward
credited PRP
for his ability to play in that game and his success with this treatment
was
discussed on national television.
|
|
|
To
Top
|
|
To
Top
|
|
|
Since
then, other high profile athletes - such as Takashi
Saito,
closing pitcher for the L.A. Dodgers, and golfer Tiger
Woods - credit PRP
for helping them return to their sport. PRP continues to
gain wider acceptance
in the sports world with studies continuing to validate
the use of PRP for ligament
and tendon injuries, knee osteoarthritis, degenerative
knee cartilage,
chronic elbow tendonosis, muscle strain and tears,
jumpers knee,
plantar fasciitis and rotator cuff tendinopathy - albeit
some skeptics
and controversy remains.
|
|
|
|
As
the use of PRP has grown the demand and availability for
smaller,
more portable and affordable machines has also
grown.
There are now several available models which allow the physician
to create PRP from a
small sample of a patient’s blood in the office setting.
Machines
are very affordable and many companies offer a complimentary
machine with a
minimum purchase of PRP preparation kits over a period of time.
However, not all marketed PRP devices are equal;
they vary
in quantity of blood required, platelet concentration,
viability and number of spin
cycles.
Harvest Technologies was one of the first PRP devices
to gain FDA approval. This system uses a floating shelf technology
which
preserves the viability of platelets until use.
In his 2005 text, Marx rated the PReP
unit by Harvest Technologies,
along with PCCS by Implant Innovations, as the two most
effective
and practical PRP devices for physician office use,
outpatient surgery
centers, and wound care center treatment.
Since then, other companies have produced additional
effective platelet concentrating systems.
|
|
|
To
Main Page
|
|
To
Main Page
|
|
|
|
|
|
Terms
& Policies
|
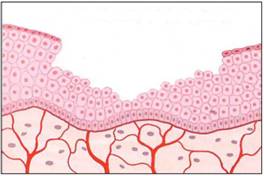
Illustration of the split thickness skin graft donor site
no PRP at
45 days.
|
To
Top
|
|
|
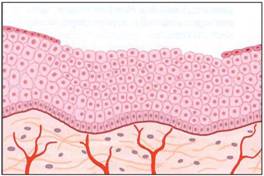
Illustration of the split thickness skin graft donor
site
with PRP
enhancement at 45 days.
|
|
|
About BMOTV™
|
|
How
To Participate in a Story
|
|
|
What
is Prolotherapy?
Prolotherapy is a nonsurgical treatment which stimulates
healing.
Short for "proliferation therapy,"
Prolotherapy is also known as nonsurgical
ligament and
tendon reconstruction, or regenerative injection therapy.
Prolotherapy
works by stimulating the body's own natural healing
mechanisms
to repair injured musculoskeletal tissue. The
treatment originated in the 1930's
when Dr. Earl Gedney, an osteopathic surgeon
successfully treated
his own severe hand injury.
Prolotherapy works by getting the body
to use its own
natural healing mechanisms to repair injured
and painful joint areas.
|
|
|
To
Main Page
|
|
To
Main Page
|
|
|
Types
of Prolotherapy:
include Dextrose
Prolotherapy, Platelet
Rich Plasma Prolotherapy
Referred to as "PRP") or bone marrow and/or fat (adipose)
tissue from an
individual's own body which contain adult stem stromal
cells
(known as Biocellular
Prolotherapy).
At the Hemwall Center these multiple
types of Prolotherapy
are done as needed to achieve the
best result.
We also use diagnostic musculoskeletal ultrasound imaging to detect
and direct
injections to the correct injury site.
|
|
|
To
Top
|
|
To
Top
|
|
|

After Blood is Separated in Centrifuge
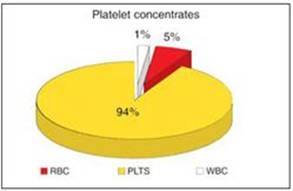
|
|
|
Terms
& Policies
|
Top
in red:
Cell
ratios in a normal blood clot: Red blood cells
(RBC),
platelets (PLTS), and white blood cells (WBC).
Bottom in Yellow
Cell
ratios in a platelet rich plasma: red blood
cells (RBC),
platelets (PLTS), and white blood cells (WBC). Bottom
Yellow
|
How
To Participate in a Story
|
|
|
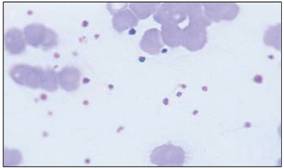
Peripheral blood smear in normal blood.
|
|
|
|
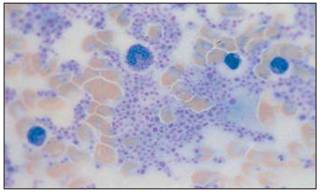
|
|
|
To
Main Page
|
A
peripheral blood smear of platelet rich plasma.
|
To
Main Page
|
|
|
|
|
|
|

THE HARVEST MACHINE
(CENTRIFUGE)
|
|
|
To
Top
|
|
To
Top
|
|
|
CREATION AND ACTIVATION OF PRP
A small amount of the patient's blood is drawn (20-120
cc) into a syringe
with a small amount of citrate (an anti-clotting
agent) then typically spun
for about 15 minutes in a special centrifugation system
that separates
the platelets, blood, and plasma.
The plasma-poor layer is then drained off and the “buffy
coat” plasma layer
is extracted along with a small amount of plasma and red cells.
In the surgical setting, PRP is activated by the surgeon mixing
in calcium
chloride and/or thrombin to make a
gel-like graft and then placing it where
he/she wants
accelerated healing.
Type I collagen has also been found to be effective
in activating and
creating a PRP graft.
In 2006, Murray et al demonstrated successful
increase in healing
of a central anterior cruciate
ligament (ACL) defect in a canine ACL using
a
collagen-platelet rich plasma matrix graft.
In some musculoskeletal studies, a 10% solution of
calcium chloride is
added to the PRP just prior to injection or is injected
simultaneously
via another syringe into the area being injected with PRP.
Activation also occurs
by exposure to tendon-derived collagen released
by the injured tissue which is being treated.
“Peppering” the tissue
during injection with
the needle tip can help ensure endogenous thrombin
release needed for activation.
Growth Factors in PRP
granules are released when
platelets
are activated.
After activation, secretion of
growth factors begins
within
10 minutes. The viability of the platelets and continued release
of
growth factors into the tissue continues for seven days.
Meantime, the platelets
stimulate the influx of macrophages,
stem cells and other repair cells, as discussed
previously.
Micro-trauma created by the injection itself also
stimulates influx
of macrophages and growth factors as in the case of dextrose
Prolotherapy.
Once the platelets die (average
life span 7-10 days), the macrophages
continue wound healing regulation by secreting some of the
same growth factors
as the platelets did, as well as others. The amount of
initial platelets present
in the wound determines the rate of wound healing
and explains why
PRP used during a surgical procedure
speeds recovery.
This may be because PRP has a strong
effect in the early phase
of healing. Use of a “matrix” such
as adipose tissue or
collagen fibers to hold the PRP material has been used
especially in the case of a large
defect.
|
|
|
To
Main Page
|
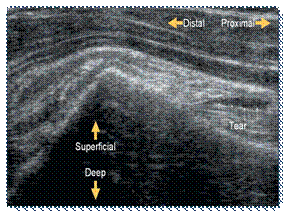
Tear of long head biceps tendon in a 70 year-old
patient
(ultrasound image)
BEFORE PRP TREATMENTS
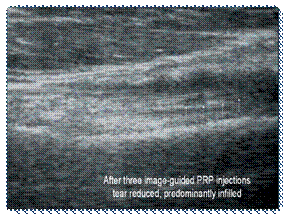
AFTER
3 PRP INJECTIONS
Resolved tear of long head biceps tendon post three
ultrasound
image-guided PRP injections.
|
To
Main Page
|
|
To
Top
|
In
our upcoming stories we will be testing
the many uses of PRP combined with Fat Transfers
to rejuvenate soft tissues and bones
in the face, gums, neck & hands.
|
To
Top
|
|
|
|
|
|
To
Main Page
|
|
To
Main Page
|
|
|
|
|
"BMOTV™
Wishes you to Look
and Feel Forever Beautiful."
|